![]()
Artificial disc
About the Artificial Disc | An Alternative to Fusion | Why It's Big News | Benefits | Drawbacks | Lumbar vs. Cervical
 About
the Artificial Disc
About
the Artificial Disc
Perhaps the most anticipated advance in spine surgery over the past 20 years is the arrival of the artificial disc, which received formal approval by the Food and Drug Administration (FDA) for widespread use in the United States on October 26, 2004.
The
artificial disc is projected to have a dramatic impact on the field
of spine, just as the introduction of the artificial joint had for
those with damaged knee or hip joints. Before the introduction of
the artificial knee or artificial hip, these joints often had to
be fused. However, thanks to artificial joint implants, thousands
of people each year regain the ability to walk. Finally, this new
technology is being brought to the field of spine.
[top]
An Alternative to Fusion Surgery
The
artificial disc represents the best alternative to date for spinal
fusion surgery. Each year in the U.S., more than 200,000 spinal fusion
surgeries
are performed to relieve excruciating pain caused by damaged discs
in the low back and neck areas. 
During a fusion procedure, the damaged disc is typically replaced with bone from a patient’s hip or from a bone bank. Fusion surgery causes two vertebrae to become locked in place, putting additional stress on discs above and below the fusion site, which restricts movement and can lead to further disc herniation. An artificial disc replacement, however, is designed to duplicate the function level of a normal, healthy disc and retain motion in the spine.
Some
experts estimate that over the next 10 years, more than half of patients
who would otherwise receive a fusion will receive an artificial disc
instead. Educated consumers nationwide are expected to migrate towards
regional spine centers of excellence for access to this latest technological
advance in spine care.
[top]
Why the Artificial Disc is Big News
 The
arrival of the artificial disc is tremendous news because of the widespread
incidence of degenerative disc disease. A natural byproduct of aging
occurs through the loss of resiliency in spinal discs and a greater
tendency to herniate, especially when placed under a heavy load, like
when we lift objects. Additionally, some people have a family history
of degenerative disc disease, which increases their risk of developing
it.
The
arrival of the artificial disc is tremendous news because of the widespread
incidence of degenerative disc disease. A natural byproduct of aging
occurs through the loss of resiliency in spinal discs and a greater
tendency to herniate, especially when placed under a heavy load, like
when we lift objects. Additionally, some people have a family history
of degenerative disc disease, which increases their risk of developing
it.
When a natural disc herniates or becomes badly degenerated, it loses its shock-absorbing ability, which can narrow the space between vertebrae. In fusion surgery, the damaged disc isn’t repaired but rather is removed and replaced with bone that restores the space between the vertebrae. However, this bone locks the vertebrae into place, which can then damage other discs above and below.
A common aspect of all artificial discs is that they are designed to retain the natural movement in the spine by duplicating the shock-absorbing and rotational function of the discs Mother Nature gave us at birth. Most artificial disc designs have plates that attach to the vertebrae and a rotational component that fits between these fixation plates. These components are typically designed to withstand stress and rotational forces over long periods of time. Still, like any manmade material, they can be affected by wear and tear.
 Manufacturers
of artificial discs aim to design discs that are not only resistant
to wearing out but that are easily replaced if revision surgery is
needed.
While artificial disc surgery is still relatively new,
the potential benefits are very encouraging for those with degenerative
disc disease.
Manufacturers
of artificial discs aim to design discs that are not only resistant
to wearing out but that are easily replaced if revision surgery is
needed.
While artificial disc surgery is still relatively new,
the potential benefits are very encouraging for those with degenerative
disc disease.
[top]
Benefits
Generally speaking, those who receive artificial disc replacements return to activity sooner than traditional fusion patients. Because there is no need to harvest bone from the patient’s hip, there is no discomfort or recovery associated with a second incision site. Some of the overall benefits of artificial disc surgery include:
- Retains movement and stability of the spine
- Prevents degeneration of surrounding segments
- No bone graft required
- Quicker recovery and return to work
- Less invasive and painful than a fusion
- Reduces pain associated with disc disease
Drawback
When treating knee and hip replacement patients, orthopedic surgeons try to postpone the implantation of an artificial joint until a patient is at least 50 years old so that they do not outlive their artificial joint, which typically lasts anywhere from 15 to 20 years. Revision surgery, which may be necessary to replace a worn-out artificial joint, can be complex.
This
is also a concern with the artificial disc. Unlike knee and hip replacement
patients who are typically in their 50s or 60s, many patients can
benefit
from artificial disc technology at a much younger age — in their
20s or 30s. Therefore, the implantation of an artificial disc in younger
patients can raise a surgeon’s concern about the potential life
span of the artificial disc in the spine and the need for revision
surgery
to replace a worn-out artificial disc, which can be complex.
[top]
Lumbar
vs. Cervical Artificial Discs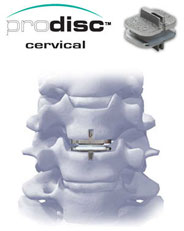
Because of the weight of the body and the rotational stress that the trunk places on discs in the low back (lumbar) area, more stress is placed on artificial discs in the lumbar area than in the neck (cervical) area, which only supports the weight of the head. Consequently, many surgeons anticipate FDA approval of new artificial discs for the cervical area, as wear and tear on an artificial disc in the neck area may be less than a lumbar artificial disc.
A second issue relates to the ease of the artificial disc surgery and any necessary revision surgery to replace a worn out artificial disc. Because the surgeon must access the front of the spine, an incision is made in the abdomen for lumbar discs and in the front of the neck for cervical discs. Generally speaking, access to the cervical discs can be easier than the lumbar discs.