![]()
Spine Surgery
When spine surgery is necessary
For some problems, surgery may be the best option. In other cases, such as a herniated disc, the physician will only recommend surgery after nonsurgical treatments like injection therapy and physical therapy has been tried without success. This is because, in some cases, the pain symptoms caused by a herniated disc can be relieved without surgery. Surgery should never be recommended for muscle-related problems.
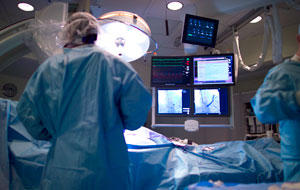
As part of their philosophy of care, physicians at Neurological and Spine Institute attempt to avoid the use of surgery unless other methods have failed or if there is danger related to delaying surgery.
If spine surgery is performed, in almost all cases, the patient will participate in post-surgical rehabilitation as part of the normal recovery process. Therapists will help the patient return to activity at a safe and prudent speed. The objective is to return the patient to full function with a strong emphasis on range of motion therapy and spine exercises.
Common Spine Surgeries
Lumbar discectomy | Cervical discectomy | Spinal fusions | Artificial disc replacement surgery | Laminectomy & laminoplasty | Corpectomy | Rhizotomy | Scoliosis surgery | Dorsal column stimulation |
Lumbar discectomy
Discectomy is the removal of the herniated portion of a disc to relieve the pressure on nearby nerves as they exit the spinal canal. Contrary to popular belief, the disc does not slip out of position like a watermelon seed. Instead, the disc is like a jelly donut, acting as the functional shock absorber between two bony vertebrae.
An injury or damage from a lifting incident may cause the jelly center to break through the wall of the disc. When the disc herniates, the jelly center can press on nearby nerves. This causes back or leg pain when the herniation is in the low back, and arm pain if the disc is in the neck area.
In a lumbar discectomy, the surgeon typically only removes the portion of the disc that is causing a problem, not the entire disc. If you have a herniated disc, keep in mind that a disc has a purpose. When you remove a disc, it may cause instability in the joint, and a surgeon may recommend a fusion to re-stabilize the area.
The surgeon can remove the damaged piece of disc through a traditional incision in the back or neck or with a surgical probe, such as in percutaneous discectomy.
Depending on the nature of your disc problem, your surgeon will recommend the most appropriate type of surgery for you.
[top]
Cervical discectomy
A cervical discectomy involves the partial or complete removal of a damaged or ruptured disc in the neck (“cervical” area). The goal of this procedure is to relieve pressure from the spinal cord or nerve roots caused by the offending disc. After the removal of the disc, space in between vertebrae may be left empty. In this case, the surgeon may use bone graft to restore the space and provide stability. The bone graft also functions to fuse the vertebrae together over time.
[top]
Spinal fusions
The goal of fusion surgery
The purpose of spinal fusion surgery is to stabilize a segment of the spine that has weakened and eliminate motion at that segment. This stabilization will ideally reduce the pain that is associated with vertebral movement.
What’s involved?
The actual process of a fusion surgery involves the insertion of bone graft into the empty space between two (or more) vertebrae. Eventually these vertebrae should "fuse" together to form a single solid segment.
Bone graft that is necessary for a fusion procedure can be attained in one of a few ways:Autograft bone – harvested from the patient’s hip
Allograft bone – harvested from a cadaver bone
Synthetic bone graft substitutes – currently being developed more extensively and expected to eventually replace other types of bone graft
Is fusion surgery right for me?
The decision whether or not to undergo fusion surgery should involve a consideration of many factors. It is important to keep in mind that fusions should be performed only if nonsurgical treatments have been explored unsuccessfully. The amount of instability and empty disc space in the spine should also be considered. Talk to your spine specialist to receive an expert assessment and feedback.
Pain caused by movement at a vertebral segment can be amplified if other conditions are present, such as degenerative disc disease, spondylolisthesis, fractures, scoliosis or a weak spine. Although fusion surgery limits movement and flexibility, it also helps to ease this pain.
Types of fusion surgery
In “anterior” spinal fusion surgeries, the spine is approached through the abdomen, and back muscles and nerves are left undisturbed. An anterior approach is taken when the spine is fairly stable and when there is a high amount of disc space to restore. The spine is approached through the lower back in “posterior” fusion procedures, which is appropriate when there is a greater amount of instability in the spine.
Lumbar spinal fusion surgery is primarily performed when only one vertebral segment is involved. Anterior and posterior lumbar fusions are frequently used in conjunction with each other, in order to provide increased strength to the fused spine.
Patients who run a higher than average risk of experiencing unsuccessful fusion surgeries include smokers and those who are clinically obese.
[top]
Artificial disc replacement surgery
In late 2004, the FDA approved the first artificial disc implant for use in the United States. While artificial disc surgery holds great promise, many surgeons feel that there are many issues to consider before recommending the use of an artificial disc. The upside is that the artificial disc promises to retain motion in the spine. The downside is that the artificial disc may wear out, requiring a complex re-do surgery.
[top]
Laminectomy and laminoplasty
A laminectomy involves the partial or entire removal of a bone segment in order to create more room for nerve roots. The purpose of a laminectomy is to relieve pain that is caused by a growth or inflammation of the facet joints, which places pressure on spinal nerves. This type of pain is often associated with spinal stenosis. A spinal fusion may accompany a laminectomy procedure to provide stability and prevent recurrences of spinal stenosis.
Similarly, a laminoplasty surgery aims at creating more space for the spinal cord and roots. Because it involves swinging one side of the lamina open like a door, this procedure is also called an “open-door laminoplasty.” Like a laminectomy, a laminoplasty is often used to treat those suffering from spinal stenosis, which involves a narrowing of the spinal canal, by relieving pressure from the spinal cord and giving it more room by increasing the diameter of the spinal canal.
[top]
Corpectomy
A corpectomy is often performed for patients suffering from all levels of cervical stenosis. The goal of a corpectomy is complete decompression of the cervical canal when stenosis encompasses more than just disc space and has moved into vertebral bodies.
Bone spurs forming toward the back of a vertebral body or the ligament behind vertebral bodies can cause the cervical spinal canal to narrow. Therefore, it may be necessary to remove one or more degenerating vertebrae and the discs above and below in order to decompress the spinal cord / nerve roots.
A corpectomy involves a vertical incision in the neck. The middle portion of the vertebra and its adjacent discs are removed to achieve decompression of the cervical spinal cord and nerve roots. A fusion accompanies a corpectomy surgery, using bone harvested from the patient’s hip or from a bone bank. This bone graft is used to reconstruct the spine and provide stability.
[top]
Rhizotomy
Rhizotomy is a procedure in which the physician may use heat or cold to intentionally damage the ability of a problematic nerve to telegraph pain signals to the brain. While pain signals serve to warn us about danger or injury, sometimes a nerve can end up in a "stuck" position, sending a continuous pain signal to the brain.
"Neuroablation" is another word used to describe the surgical procedure to purposely inhibit the nerve's ability to transmit a pain signal. During the procedure, the spine surgeon can destroy the problematic nerve by cutting it or by using extreme heat or cold. This intentional "short circuit" can be temporary or permanent, depending upon the procedure.
Trying to mask this signal with drugs can have damaging long-term implications. Drugs can have dangerous side effects to internal organs. By using rhizotomy, the pain signal is turned off at the source.
[top]
Scoliosis surgery
Through the placement of hooks, rods and screws, a spinal curve can be corrected and stabilized. A fusion often follows scoliosis surgery, in order to maintain the correction permanently.
Scoliosis is not the result of an injury and usually appears without cause. It can be inherited, and it usually affects more women than men. In the case of most spinal curves, the spine is not only bent but twisted like a corkscrew.
Some cases of scoliosis are not serious. Over time, if a curve worsens, surgery may be required to correct it. In extreme cases in which the curve is not corrected, spinal deformity can place pressure on internal organs and shorten a person's life expectancy.
During scoliosis surgery, the surgeon may use special instruments that hook onto various vertebra segments. These surgical rods are the adjusted to "de-rotate" the twisted and bent corkscrew.
Decades ago, Harrington Rods were used to surgically straighten the spine. However, this technique did not untwist or correct the spine. Current state-of-the-art instrumentation achieves much better spine correction than older rods did.
Generally speaking, the younger the patient, the more flexible the spine and the better the result from scoliosis surgery. As the patient becomes older, say over 40 years old, the spine is less flexible, and there may be a greater risk involved in attempting to correct the curve. Because the spinal cord is involved, only spine surgeons who specialize in scoliosis should perform scoliosis surgery.
[top]
Dorsal column stimulation
Dorsal column stimulation, also known as spinal cord stimulation, is used in complex cases of back pain that cannot be resolved nonsurgically or with another surgery. In most cases, it is used when leg pain is worse than back pain. The intent of dorsal column stimulation is to use an electrical signal instead of drugs to mask pain that cannot be removed any other way.
During this procedure, the patient is awake, and the surgeon delicately places tiny electrodes under the skin in the back. At that point, a tiny electrical current is transmitted through the wires to the desired location in the back. This sensation feels like a tiny tickle, as the electrical current interrupts the pain signal that may be sent to the brain from the damaged nerve. The patient helps instruct the surgeon as to which electrical setting and placement of wires produces the most pain relief. It is important to note that this technique is only used in the most extreme cases of back and leg pain.
[top]